Upstate Vet Emergency & Specialty Care (UV - Greenville)


Our Commitment
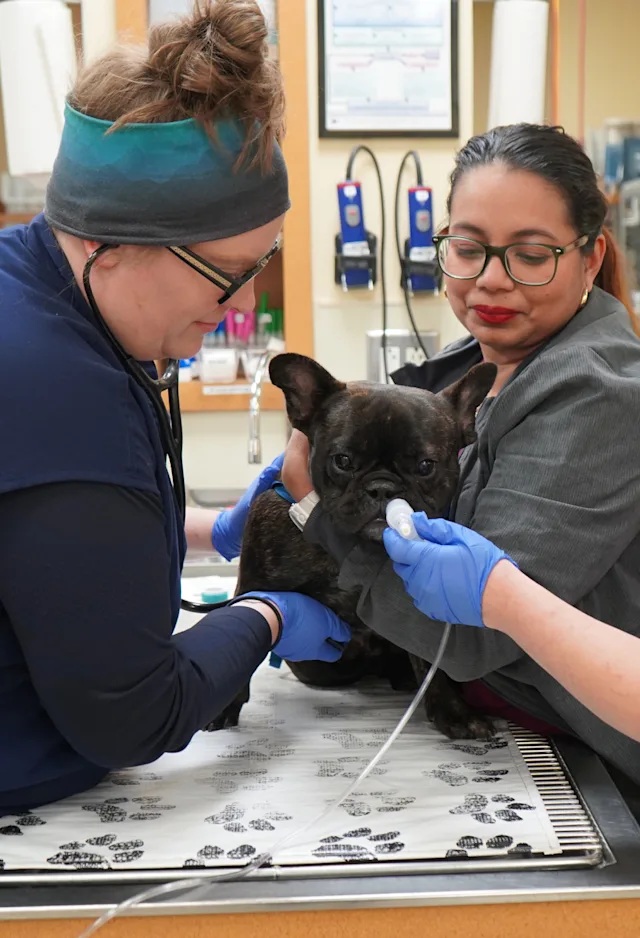
At Upstate Vet we understand that pets are members of the family. Our dedicated team of doctors and medical staff are consistently pushing to offer our patients the best in diagnostic and advanced medical care. As a referral animal hospital, we work closely with your family veterinarian to provide your pet with a complete healthcare team. You can rest easy knowing that your pet is in the most capable hands at Upstate Vet.
Client Reviews & Testimonials
We value feedback from our clients. Here is just a small sample of the hundreds of happy and healthy pets that we have cared for.
★★★★★
They have an amazing staff! They are very knowledgable, compassionate and truly care about animals and their owners. Ross had to spend the night and was taken good care of during his stay. They called me with updates and provided a plan that helped him recovery quickly so he could get back to doing the things he loves. Dr. Rathke and the entire staff are wonderful! Thank you all!
Cathy G.
★★★★★
Dr. Martinez and his team went above and beyond with our German Shepherd, Ringo. We brought Ringo in February and received the devastating news of cancer. Dr. Martinez took the time to cover all our options. The treatment plan we chose put Ringo in complete remission and we were ecstatic when we got to ring the bell!
Tracy H.
★★★★★
We saw Dr. V with our dog that has chronic kidney disease. She was excellent and thoroughly explained the condition, tests done, plan and follow up. Her team is also very kind and helpful. Their care is outstanding!
Debra M.