![]()
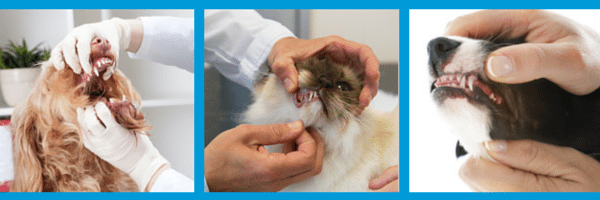
According to the American Animal Hospital Association nearly two-thirds of pet owners do not provide the dental care recommended by their veterinarians. Therefore, it is no surprise that 85% of dogs and cats over the age of 3 will have periodontal disease. Progression of the disease involves the interaction of the host’s defense mechanism with the numerous gram positive aerobes and gram negative aerobes in plaque. The good news is that periodontal disease can be reversed if treated in the early stages. Unfortunately, advanced stages of the disease are irreversible and typically require removal of affected teeth or more advanced therapy such as bone grafting. Let’s start our discussion on treatment by defining the different stages of Periodontal Disease –
Stage 1: Gingivitis only, no loss of periodontal ligament attachments
Stage 2 : <25% loss of periodontal ligament attachments, early radiographic changes of bone resorption Stage 3 : 25-50% loss of periodontal ligament attachments, beginning to see slight exposure of furcation of tooth roots Stage 4 : >50% loss of periodontal ligament attachments, with significant furcation exposure
Stage 1: Most patients with stage 1 PD can be managed with a home care regimen. Daily brushing is considered the “Gold Standard” of dental home care. I typically recommend an enzymatic/non-fluoride flavored toothpaste such as CET and a soft bristl the tooth brush. For pets that will not tolerate brushing, a weekly plaque prevention gel such as Oravet (for pets with more advanced periodontal disease, this should be started after a dental prophylaxis), tested dental treats, and an oral hygiene water additive such as Dog:Essential Healthymouth are good alternatives.
Stage 2: Professional Dental Cleaning with Dental X-rays, followed with the daily home care recommendations of daily tooth brushing, water additives, dental treats and plaque prevention gels.
Why are dental radiographs so important in veterinary dentistry?
Radiographs will not only provide a much more objective evaluation of the severity of periodontal disease but have also been found to reveal additional pathology in approximately 50% of patients, pathology that is not apparent on visual examination.
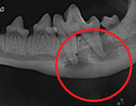
Dead and abscessed tooth
Stage 3: Professional Dental Cleaning with Dental X-rays, +/- Periodontal Therapy, followed with the daily home care recommendations of daily tooth brushing, water additives, dental treats and plaque prevention gels.
Periodontal Therapy: (Doxirobe therapy vs. bone grafting)
Pockets 4mm or less: While it is important to get these teeth cleaned, disease will often progress if we do not also consider periodontal therapy. Periodontal pockets measuring 4mm or less should be thoroughly cleaned with an ultrasonic scaler using a periodontal tip and/or cleaned with a hand curette. I then apply a periodontal-specific antimicrobial such as Doxirobe gel which is a slow release form of Doxycycline. Once applied, the gel will harden into the consistency of a wax candle and remain in the pocket for about 45 days. In this way it not only fights infection and inhibits tissue destruction but it prevents debris and plaque from filling up the defect.
Pockets greater than 4mm: Because these pockets are so deep a gingival flap must be created adjacent to the pocket in order to allow sufficient visualization for scaling, cleaning and periodontal therapy. If the pocket is >4mm and there is enough surrounding alveolar bone to support placement of a bone graft, then bone grafting is recommended. There are many different types of bone grafting products available for advanced periodontal therapy. Please feel free to contact me with any questions you have on any of those products. After the pocket has been thoroughly cleaned and bone graft has been placed, the flap is replaced and sutured using a 5-0 monofilament dissolvable suture.
Stage 4: Many of our patients, unfortunately, will have some of their teeth that have progressed to this level by the time we see them and in these cases the only real option is to extract the affected teeth.
Visit here for tested & approved veterinary dental treats & products: www.VOHC.org
This is probably the second most common lesion we will see on a routine dental exam/cleaning.
The vitality of any tooth depends on the viability of the pulp(the blood vessels and nerves of that tooth). The dental pulp has fingerlike projections that extend into the microscopic dentin tubules of the teeth. When there is pulp exposure, these vital structures are exposed to bacteria and the subsequent exposure will eventually cause the tooth to die. If the patient is 2 years of age or younger and the fracture occurred less than 48 hours prior to presentation the tooth can potentially be saved with a vital pulpotomy. This involves removal of the coronal 5mm of pulp, essentially resecting the infected portion of pulp. A pulp dressing is then placed over the healthy pulp to allow for dentin bridge formation over the exposed pulp cavity and healing. A composite restoration (“filling”) is then placed to prevent microleakage of bacteria into the treated tooth. It is important to remember that these recent fractures are a true dental emergency as we can hopefully save the tooth.
If the patient is older than 2 years of age and/or the fracture is older than 48 hours then vital pulpotomy is unlikely to be successful and either root canal therapy or extraction is indicated.
Root Canal Therapy:
When performing root canal therapy all of the infected pulp tissue is removed using endodontic files of gradually increasing sizes. Once the canal is cleaned a sealant is used to seal the dentin tubules and prevent bacterial penetration into the tooth, and then the pulp cavity is filled with a resin called gutta percha. A composite restoration (filling) is then placed to seal the end of the pulp cavity preventing further contamination with bacteria. A titanium crown may or may not be placed depending on the tooth affected, the cause of the fracture, and the lifestyle of the pet.
Surgical Extraction:
Surgical extraction may be the recommended treatment if:
1. The tooth is not a strategic (functional) tooth such as a canine tooth and/or carnassial tooth (maxillary 4th premolar and the mandibular 1st molar) or
2. The tooth with pulp exposure has advanced periodontal disease (in this case extraction may be a better option), or
3. The owner has financial constraints.
Helpful hints for surgical extractions:
• Mucogingival flaps allow for much better exposure of the tooth root and closure of the gingival void after tooth extraction. When creating a mucogingival flap it is important that the flap is wide enough for closure and will have no tension upon suturing. Leaving a surgical site open can lead to delayed or non-healing at that site with subsequent painful osteonecrosis (dry socket).
• Have the right tools for the job!
Periosteal Elevators: Helps in releasing your mucogingival flap
• High-speed Hand Piece: It is crucial for it to have copious water flow
• Proper Sized Burs: The burr sizes I commonly use are # ¼ round, # 2 round, and #557 cross cut fissure burs. It is important to remember that burrs dull very easily and should only be used on one patient.
• Dental Elevators and Luxators: It is very helpful to have multiple sizes and to ensure that they are sharp and sterile.
• Proper Suture and Needle Sizes: A dissolvable monofilament suture is recommended. I like using 5-0 monocryl with a P3 reverse cutting needle for smaller patients and 4-0 monocryl with a FS-2 reverse cutting needle for larger patients.
• Once the mucogingival flap is released and retracted from the extraction site, the overlying alveolar bone is removed using a cutting burr on a high-speed hand piece with copious water flow (you may remove up to 75% of the alveolar bone along the buccal aspect if needed)
• Once the overlying alveolar bone has been removed and the tooth root is visible, the periodontal ligament is cut using a #1/4 round bur
(holding the bur parallel to the tooth in the areas of the periodontal ligament spaces)
• If the tooth is multi-rooted, the tooth must be divided into its respective crown-root sections before elevating.
• Now you are ready to elevate using dental elevators or luxators
• When the tooth is mobile enough to remove with your fingers, you may use the extraction forceps to remove the tooth from its alveolus.
• After removing the root it is important to ensure that there are no sharp areas of alveolar bone that could cause subsequent pain. • Any remaining sharp areas can be eliminated using a burr.
• Don’t forget your postop dental radiograph to show complete removal (not only does this help with knowing how you’ve done but it is also part of the legal medical record)
• Create a tension free mucogingival flap (by releasing the periosteal layer) and suture in place using simple interrupted sutures placed ~2mm apart.
**What happens if the tooth breaks and there is a retained tooth root?**
The retained tooth root should be treated just as you would any other tooth. Begin by removing more buccal alveolar bone, as needed, with a #2 round bur so the root can be visualized. A #1/4 round bur can then be used to cut along the periodontal ligament spaces. Elevate using an elevator of appropriate size for the root involved.
**Side note: It is important to avoid the temptation to “pulverize” roots using a dental burr. Not only does this interfere with your ability to visualize the extraction site, but it can cause tremendous thermal damage to the surrounding alveolar bone and tissues.
Even though the pulp cavity is not exposed these fractures should also be evaluated carefully as the microscopic dentin tubules that extend from the pulp into the tooth may have become exposed. This means that bacteria can still enter the pulp cavity. Additionally, exposed dentin can also be very painful to the patient (just like in humans). These teeth with uncomplicated crown fractures should have dental radiographs taken to evaluate for any evidence of endodontic disease (make sure the tooth still appears vital).

Once it is determined the tooth is vital, an adhesive bonding (sealant) can be applied. This adhesive bonding actually creates micromechanical bonding inside the dentin tubule, sealing them off and preventing bacterial entry in the future.)
We hope you find this information helpful as you manage your dental patients. We have included some resources below that you may also find useful. Please let us know if Dr. Duncan can help you in any way as you continue to develop the dental component of your practice. Dr. Duncan is available by email (hduncan@uvs.cc) and phone (864-233-7650) for any dental questions.